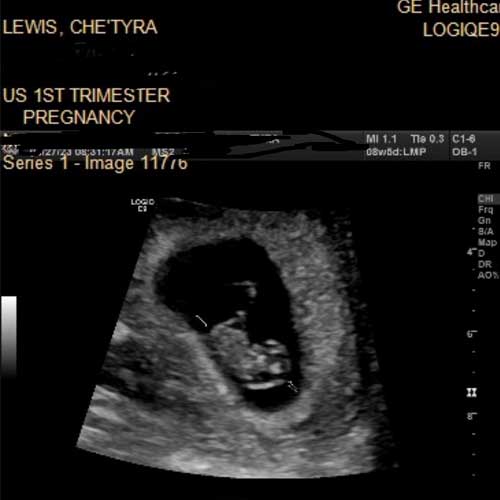
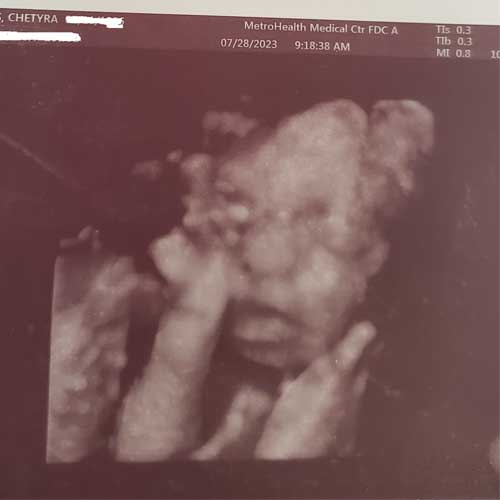
An ultrasound at around 22 weeks revealed Che’tyra Lewis was having a boy. It also showed something else: Her cervix looked short, which increases the risk of pregnancy loss, preterm labor and premature birth
“MetroHealth didn’t just take me on as a patient, they cared for me as a human being”
In June 2023, an ultrasound at around 22 weeks revealed Che’tyra (“Ché”) Lewis and her boyfriend, Marcus Williams, were having a boy. It also showed something else.
Jessica Pippen, MD, a maternal-fetal medicine physician who specializes in high-risk pregnancies at MetroHealth, reviewed the results: Ché’s cervix looked short, which increases the risk of pregnancy loss, preterm labor, and premature birth.
“When she left the room, I was in my boyfriend’s arms literally crying,” Ché said.
Ché’s pregnancy was too advanced for a cervical cerclage, a stitch that reinforces the cervix. So, after having a full exam to make sure she and her baby were healthy, Ché was sent home with instructions to go on light duty. That meant not carrying more than 10 lbs., and no vigorous walking.
On July 7, Ché returned for a follow-up with a high-risk OB-GYN nurse practitioner, Emily E. Biehl, DNP, APRN-CNP.
Brian Mercer, MD, another maternal-fetal medicine specialist, stopped by to consult. He told Ché her cervix had gotten significantly shorter over the past week. She wasn’t leaving the hospital.
“We had just gotten used to being pregnant, and then – boom!” Ché said. “I felt really insecure, and I felt like I had no choice but to have faith. I literally had nothing else.”
It was tough news for Ché, who had started a new job with health insurance the day before. She and Marcus were busy moving into a new home.
Four hours later, Ché met the doctor on call, Kelly S. Gibson, MD, MetroHealth’s Division Director of Maternal Fetal Medicine. It was a Friday, so Ché thought she might only have to stay for the weekend.
On Monday, Dr. Gibson told Ché she’d need to stay in the hospital until she delivered or until she reached 28 weeks, whichever came first. Chances were high she could go into preterm labor. Ché was only 24 weeks pregnant.
“We were very afraid that she would quickly deliver,” Dr. Gibson said.
It was a roller coaster of emotions for the couple. “We’ve known each other a long time, but we’d only been a couple for a few months,” Marcus said. “I was worried about them, and the baby not making it.”
Doctors limited the amount of time Ché spent outside of her room. Sue Baker, RN, made sure the window blinds were opened every morning and arranged for visits from an art therapist.
Social worker Kelly Gareau helped Ché navigate the Medicaid application process while waiting for her health insurance to kick in. Dr. Gibson checked in daily.
Ché toured Labor and Delivery, the NICU, and postpartum rooms.
“MetroHealth didn’t just take me on as a patient, they cared for me as a human being,” she said.
Ché reached 28 weeks and went home on August 8. Although she was put on bed rest and had weekly ultrasounds and appointments with Dr. Gibson, Ché squeezed in a few weeks of work. Her new boss had held the job for her.
On October 22, Ché attended her baby shower. The next day, Dr. Gibson gave Ché the option of having labor induced that night – not only because Ché was dealing with dizziness, labored breathing, and an elevated heart rate but to ensure that she was on call and available for the delivery.
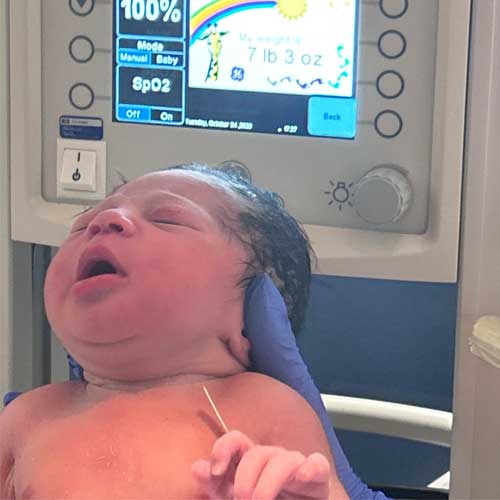
Ché had made it to 40 weeks. On October 24, she gave birth to Marcus Jr. (MJ). He was 7 lbs. 2 oz. and 21 inches. They were home two days later.
“Had you told me that this would be the outcome when I first met her, I’m not sure I would have believed it,” Dr. Gibson said. “Ultimately, she did really well. She stayed positive through it all.”
Today, MJ is almost 6 months old. “He’s a full-blown Scorpio, small and sassy,” Ché says.
Ché says she’s grateful for her time at MetroHealth and the team involved in her and MJ’s care. “Every person at MetroHealth fought for me so hard. My baby literally had a team of people every single day.”
She and Marcus have talked about the future. “If we do decide to have more children, I will go right back to Dr. Gibson for every baby, from now on.”
Maternal-Fetal Medicine Specialty Clinics
MetroHealth offers several specialized clinics and programs to address specific concerns during pregnancy.
To make an appointment regarding high-risk pregnancy issues, call the Maternal-Fetal Medicine department at 216-778-4444.